Although the disease is not highly contagious, the Department of Health (DOH) warned that meningococcal meningitis can kill in a matter of hours.
The DOH said that meningococcemia, caused by the neisseria meningitidis bacteria, can spread through direct contact with discharges from the nose and throat.
The Geneva-based World Health Organization (WHO) has reported that a variety of organisms, including different bacteria, fungi or viruses, can cause meningitis. Meningococcemia can cause severe brain damage and is fatal in 50 percent of cases if untreated.
Meningococcal disease has two common outcomes—meningitis and bloodstream infection. The United Nations health agency says there are 12 types of n. meningitidis, six of which can cause epidemics. Outside the human body, these fragile bacteria cannot survive in natural conditions.
These infections typically appear within three to seven days after being exposed to the bacteria. Both of these conditions are very serious and can be deadly. In fatal cases, deaths can occur in as little as a few hours. People who recover from meningococcal disease can have lifelong complications.
According to Dr. Lulu Bravo, professor emeritus at the University of the Philippines-Manila College of Medicine, meningococcemia can be so severe as to cause death within 24 hours after initial onset of fever and purpuric rashes (purplish spots caused by bleeding tiny blood vessels beneath the skin’s surface).
It has been established that meningococcal disease is transmitted only through droplets of respiratory or throat secretions from carriers (such as kissing, sneezing or coughing on someone or living in close quarters).
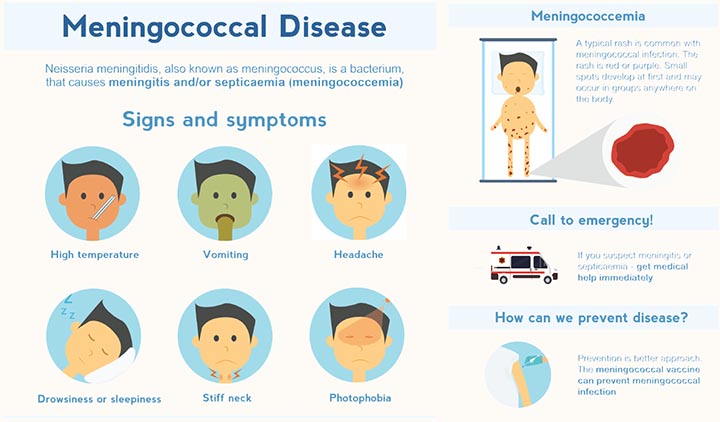
According to health experts, when the bacteria infect the meninges—the membranes around the brain and spinal cord—it causes meningitis. Widely feared by parents, meningitis is easily recognized. Symptoms of meningococcal meningitis include sudden onset of fever, headache, and stiff neck. There can be additional symptoms, such as: nausea, vomiting and confusion.
The WHO reminded the public that during the dry season between December to June, dust winds, cold nights and upper respiratory tract infections combine can damage the nasopharyngeal mucosa, increasing the risk of meningococcal disease.
At the same time, transmission of neisseria meningitidis may be facilitated by overcrowded housing. This combination of factors explains the large epidemics, “which occur during the dry season in the meningitis belt.”
In the agency’s 2012 compilation of health advisories, the DOH stressed that it is “an acute and potentially life-threatening bacterial infection of the bloodstream.”
“The bacteria frequently live in a person’s upper respiratory tract without causing visible signs of illness. [They] can be spread from person to person through respiratory droplets from coughing, sneezing, kissing, or sharing foods, drinks and utensils,” the DOH said. Even DOH Assistant Secretary Eric Tayag cautioned that about 5 percent of healthy persons harbor the bacteria. The symptoms of meningococcemia include:
- high fever
- headache
- stiff neck
- drowsiness
- dizziness
- convulsions
- vomiting
- unstable vital signs
- coughing
- rashes (rashes associated with meningococcemia are purple and, unlike other rashes, do not turn white when pressure is applied).
Children are more vulnerable to the diseases because of their low resistance to the bacteria. People of all ages can be affected and that 5 percent to 15 percent of those with meningococcemia die within 24 to 48 hours. In 2013 the DOH reported that a six-year-old boy in Quezon City succumbed to the disease two days after exhibiting symptoms, while a four-year-old girl in Sorsogon also died after showing symptoms of meningococcemia.
Following the death of a four–year-old boy being treated in Amang Rodriguez Memorial Medical Center, in the same year, the Marikina City adopted “protective” measures against the disease . The DOH advises following these measures to avoid getting the disease:
- Wash hands frequently with soap and water;
- Avoid close contact with meningococcemia patients;
- Increase resistance by maintaining a healthy lifestyle—including a nutritious, well-balanced diet, regular exercise, adequate rest and sleep, and avoiding tobacco and alcohol;
- Maintain a clean environment;
- Do not share utensils, cups, waterbottles, lipstick, cigarettes, musical instruments with mouthpieces, mouth guards, or anything else that has been in the mouth of an infected person;
- Avoid crowded places;
- Aggressive antibiotic treatment is usually given considering the case-fatality ratio of meningococcal disease is estimated to be between 10 percent and 15 percent, and even higher in the Philippines (case-fatality ratio of meningococcemia is more than 50 percent).
Vaccination
According to the WHO, vaccination is one of the most effective ways to protect yourself from getting the disease.“The vaccine is remarkably safe,” the WHO said. It added that licensed vaccines against meningococcal disease have been available for more than 40 years. “Over time, there have been major improvements in strain coverage and vaccine availability, but to date no universal vaccine against meningococcal disease exists. Vaccines are serogroup specific and confer varying degrees of duration of protection,” the WHO added.
“The WHO is committed to eliminating meningococcal disease as a public health problem,” the WHO stressed. Vaccines against infectious meningococcal disease have been available in the Philippines for more than a decade already.
In 2009 the Philippines reported 77 cases of Meningococcal disease resulting to 17 deaths. The highest incidence is noted in the age group of one to four years old with a high case fatality rate of 28 percent. The DOH said that in the recent years, the Philippines has seen many outbreaks of emerging infectious diseases and it continues to be susceptible to the threat of reemerging infections such as leptospirosis, dengue, meningococcemia, tuberculosis, etc.
The current situation emphasizes the risks and highlights the need to improve preparedness at local, national and international levels to properly address future pandemics.
“New pathogens will continue to emerge and spread across regions and will challenge public health as never before signifying grim repercussions and health burden. These may cause countless morbidities and mortalities, disrupting trade and negatively affect the economy,” the DOH noted.
Meningococcemia is compensable
The Health secretary, meanwhile, had announced that the Philippine Health Insurance Corp. (PhilHealth) will compensate the victims of meningococcemia under the government’s health-insurance program. Duque said that meningococcemia is compensable since it is considered a catastrophic case that could cause sudden death under the PhilHealth rules.
Those PhilHealth members who suffer from meningococcemia are entitled to P400 daily in room and board coverage and up to P16, 000 worth of medicines during their period of confinement adding that there are 1,500 accreditedPhilHealth hospitals and clinics where its members could go to seek treatment.
“Any member who will be confined in any PhilHealth-accredited hospital due to meningococcemia need not worry because we will cover part of their hospitalization expenses,” Duque said in a statement. He urged non-PhilHealth members to enrol in the government’s health-insurance agency in order to avail themselves of health-care benefits in the event they are afflicted with a severe ailment.
April 24 marks the World Meningitis Day, a day set to appreciate patient stories, raise awareness of the signs and symptoms of the disease and encourage vaccination to prevent further cases. The Philippine Foundation for Vaccination will spearhead the joint celebration of World Meningitis Day and World Immunization Week on April 24 at the Quezon City Memorial Circle. Everyone is welcome to take part in the celebration which will start at 6 a.m. Fun run and Zumba are just among the activities in the celebration.