Every day, cervical cancer kills 12 Filipino women. To think, the deaths could have been avoided and prevented. As a matter of fact, there is now a vaccine available against the disease. More important, cervical cancer can be cured—if detected early!
Cervical cancer is women’s enemy No. 2. “In the Philippines, cervical cancer remains as the second-most common cancer affecting women after breast cancer. It is also the second leading cause of cancer death in women,” said Dr. Salvador Villanueva, a fellow of the Society of Gynecologic Oncologists of the Philippine and the Philippine Society for Cervical Pathology and Colposcopy.
While cervical cancer incidence and deaths have been on the decline in highly industrialized countries like the United States and those in Europe, the incidence of cervical cancer in the Philippines, on the other hand, remains high.

Between breast cancer and cervical cancer, the latter is deadlier. займ на карту. In her Inquirer column, Rina Jimenez-David, a recognized advocate in reproductive health, explained it this way: “While breast cancer is the most common form of cancer for women in the country, it is not the most deadly. The death toll from cervical cancer is higher than for breast cancer, and this is mainly because by the time its victims come for treatment, it is already too late.”
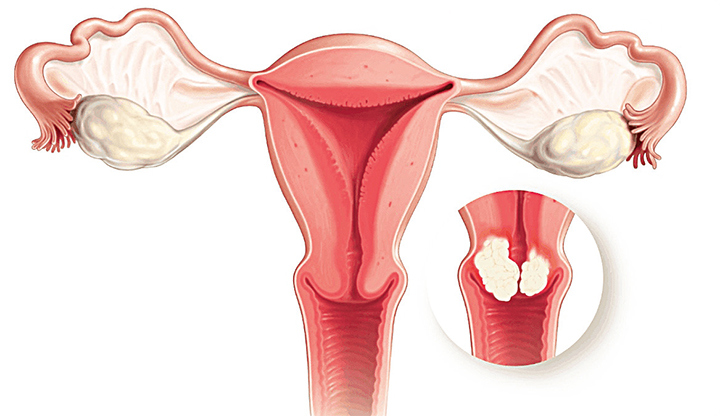
The cervix is the lower part of the uterus. It extends into the vagina. Cervical cancer, which results from the uncontrolled growth of severely abnormal cells in the cervix, usually affects women aged 35 to 55, but it can affect women as young as 20.
According to Villanueva, one of the reasons cervical cancer remains high in the Philippines is because of the many misconceptions about the disease that only a few Filipino women undergo regular screening with Pap smear and HPV (human papillomavirus) vaccination, two of the most proven ways to prevent cervical cancer.
In an article he wrote for Health and Lifestyle, a monthly publication for health professionals, Villanueva tries to segregate the myths from the facts about cervical cancer:
- Myth: Cervical cancer is caused by genetic factors, just like the other cancers.
- Fact: Cervical cancer is caused by infection with the HPV, which is easily passed during sexual contact or even through genital skin to skin contact, without penetrative sex. In fact, 99.7 percent of women with cervical cancer are positive for HPV. Condoms may reduce the risk but are not fully protective.
- Myth: Cervical cancer affects only those women with multiple sexual partners.
- Fact: Every two minutes, a woman dies because of cervical cancer. In the Philippines, incidence starts rising at the age of 35, affecting Filipinas when they are still very productive, maybe just started their families, while their children are still young or at the peak of their careers.
Women with multiple partners is just one of the risk factors. Other risk factors include: women who have a partner with multiple partners (regardless if past or present), previous history of HPV or sexually transmitted infections, smoking, early sexual activity, women who are immunocompromised or on steroids, and use of the oral contraceptive pills.
- Myth: Since there are no symptoms of vaginal bleeding or discharge, a woman need not to have a Pap smear.
- Fact: There are no early signs or symptoms of cervical cancer. HPV infection of the cervix at the start has no signs or symptoms—no fever, no discharge, no bleeding. So, a woman does not know if she has or does not have HPV infection. She has to go for regular screening by Pap smear every one to two years.
- Myth: Pap smear and HPV vaccination are painful and very expensive.
- Fact: The Pap smear procedure lasts only five to 10 minutes and it is not painful at all. The cost for the Pap smear varies from about P700 to P2,500, depending on the type of the Pap smear, the conventional or the liquid-based.
As for the HPV vaccine, all Filipinas are recommended to get the HPV vaccine, as early as 10 years of age. The cost of the HPV vaccine varies depending on the type, the doctor, and the hospital or clinic where one gets the vaccine. The price range varies from P2,500 to about P7,500 per vaccine.
- Myth: There is no hope against cervical cancer.
- Fact: There is hope against cervical cancer if treated early. Survival rates are 85 percent to 90 percent for stage 1 cancer, and 70 percent for stage 2 cancers. But survival rates go down to about 30 percent for stage 4 cancers. Treatments such as surgery, chemotherapy and radiotherapy are available and accessible in the Philippines for patients with cervical cancer.
- Myth: The best time to get the HPV vaccine is when a woman is older or when married.
- Fact: As early as 10 years old, 15 Filipinas are recommended to get the HPV vaccination. It is beneficial for every Filipina to get one as it reduces suffering and death of women, and the grief and financial burden felt by the patients’ families. It is best to have the vaccination before sexual activity starts so that one develops antibodies to the HPV virus before sexual activity might infect one. However, even if one is older, vaccination still offers some protection against cervical cancer although less if compared to the protection if vaccination was done earlier.
“Screening and vaccination are our best hope in preventing this cancer,” Villanueva pointed out.
Industrialized countries, like the United States, have achieved success in early detection of pre-cancerous conditions in the cervix with the Pap smear. But in developing countries like the Philippines, visual inspection with acetic acid (VIA) is recommended.
In VIA, a swab cotton is immersed in acetic acid, and then placed on the cervix. If an area turns whitish, this is an indicator for health practitioners to suspect for the presence of cancer.
Several international medical societies and health governing bodies have rated VIA as equally, if not more useful than Pap smear and as more appropriate and cost effective in low resource areas. In the Philippines, studies show that Pap smear has a cancer sensitivity rate of 30 percent to 89 percent, while VIA has a sensitivity of 51 percent 77 percent.
“Twenty percent of all cancers are caused by viruses,” said Prof. Ian Frazer, a clinical immunologist and currently the chairman of the Australian Cancer Research Foundation’s Medical Research Advisory Committee. “If we know that cancer is caused by a virus, then we know how to prevent it.”
And this, he added, is where vaccines would come in. “Presently, there are three vaccine brands recognized by the [government] as licensed manufacturers of the HPV vaccine,” Villanueva said. “These are the bi-valent, quadri-valent and the nano-valent HPV vaccines, all of which are proven vaccines to prevent cervical cancer.”
According to Villanueva, it is important to take three doses of HPV vaccination to ensure its maximum effectiveness. “Although, women between age 10 to 15 years may only have two doses, at least six months apart,” he said.
In a lecture held at the College of Medicine auditorium at the University of the Philippines in Manila some years back, Frazer reiterated three things that must be done when dealing with cervical cancer.
He said that a woman must undergo prevention (changing one’s lifestyle or avoid certain environments), then early detection through screening, and finally definitive therapy once the cancer cells develop.
“We have got good treatments for cervical cancer especially if we detect it early, in which state it becomes definitely curable. This is why screening is very important,” Frazer explained. “The problem arises if a woman waits until she finds she is sick of cervical cancer, wherein by that time, the disease is so advanced that is already becomes incurable.”
Image credits: WWW.FREEPIK.COM



































